CPR for the Elderly: Survival or Suffering?
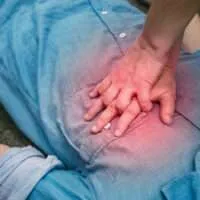
The famous life-saving rescue technique, Cardiopulmonary Resuscitation (CPR), could be worse than death, especially for the elderly. The misconceptions surrounding the use of CPR stems from the unrealistic high success rate of CPR shown on television to add a heroic plot line. In reality, CPR may cause more harm than good, with an out-of-hospital cardiac arrest survival rate of 7.6%. This rate decreases in older patients, with an out-of-hospital CPR survival rate of 6.7% in patients in their 70s, to under 3% in patients in their 90s.
When considering between life or death, logically it seems that receiving CPR is better than not, right? Unfortunately, when it comes to CPR, it is not just a matter of life or death, but an issue of a person’s quality of life, should they even survive. CPR is invasive in nature, involving painful chest compressions that could lead to serious injuries, such as cracked ribs, pulmonary hemorrhage, or brain damage. Once the body goes into cardiac arrest and the heart stops beating, the brain begins to perish immediately, with the rest of the body slowly following. Almost 30% of survivors of in-hospital cardiac arrest will face significant neurologic disabilities. Again, this rate drops significantly in older patients, with only 2% of patients over the age of 85 escaping significant brain damage after cardiac arrest and resuscitation.
It is important for every person to make cognizant choices, while one can, regarding circumstances on where they would like medical professionals to keep trying, or when it’s time to cease action. A Living Will is a document that allows an individual, known as the “principal” to make their wishes known about certain lifesaving or life-prolonging measures. Anyone over the age of 18 and of sound mind has the right to express which medical procedures they would want to be withheld at the end of life. This legally binding document outlines the principal’s wishes regarding resuscitation, life support, and organ donation. This document works in tandem with other healthcare documents. In Florida, there are several health care related documents that are recommended:
Living Will: A Living Will is a legal document that lays out a principal’s wishes for end-of-life care. A Living Will allows the individual to express their preferred medical treatment preferences and what life-sustaining measures may be taken if their death is imminent, they have an end-stage condition or are in a persistent vegetative state. It is enacted only when either one or two physicians determine that the principal is unable to make their own medical decisions. A Health Care Surrogate Designation can allow the principal to appoint an agent to make end-of-life decisions for them if they become unable to decide for themselves. The agent, called a “surrogate” has a legal responsibility to honor the principal’s wishes made in the Living Will. If an individual has not appointed an agent to execute their wishes, then the principal’s primary care physician will proceed pursuant to the wishes outlined in the person’s Living Will. Creating a Living Will can relieve family members from the agonizing decision of whether to continue or commence life-sustaining treatments.
Health Care Surrogate: A Health Care Surrogate Designation, sometimes referred to as a Medical Power of Attorney or Advance Health Care Directive, allows an individual to appoint a trusted agent to make medical care decisions on their behalf. This document can be effective immediately or effective once the principal’s primary care physician determines they are unable to make health care decisions for themselves. Although this document includes instructions about any treatment an individual does or does not want, it is crucial to discuss those wishes with the appointed surrogate.
Do Not Resuscitate Order: The Do Not Resuscitate Order (DNRO), also known as a “DNR”, is a medical order signed by a physician instructing doctors and care providers to refrain from performing CPR if an individual’s heart stops beating. The DNR ensures that resuscitation may be withheld by an emergency medical professional. This document must be signed by a physician and the principal or his or her surrogate, and printed on yellow paper. A medical professional must see this document to withhold resuscitation, otherwise, they are duty-bound to attempt life-saving measures.
As important as an Advance Health Care Directive is, it is just as important that it is kept in an accessible place and that one’s surrogate, family, and physician have a copy of it. Just like any other estate planning document, people should review and update them periodically.
SAMUELS WOOD PLLC wants to ensure you feel empowered to make your wishes known. Our lawyers have a wide range of knowledge and experience in elder law that can shield your wishes and estate. To discuss your situation with an experienced legal professional, contact our firm or call (561) 864-3371.
SOURCE:
https://www.npr.org/sections/health-shots/2023/05/29/1177914622/a-natural-death-may-be-preferable-for-many-than-enduring-cpr?f=191676894&ft=nprml

